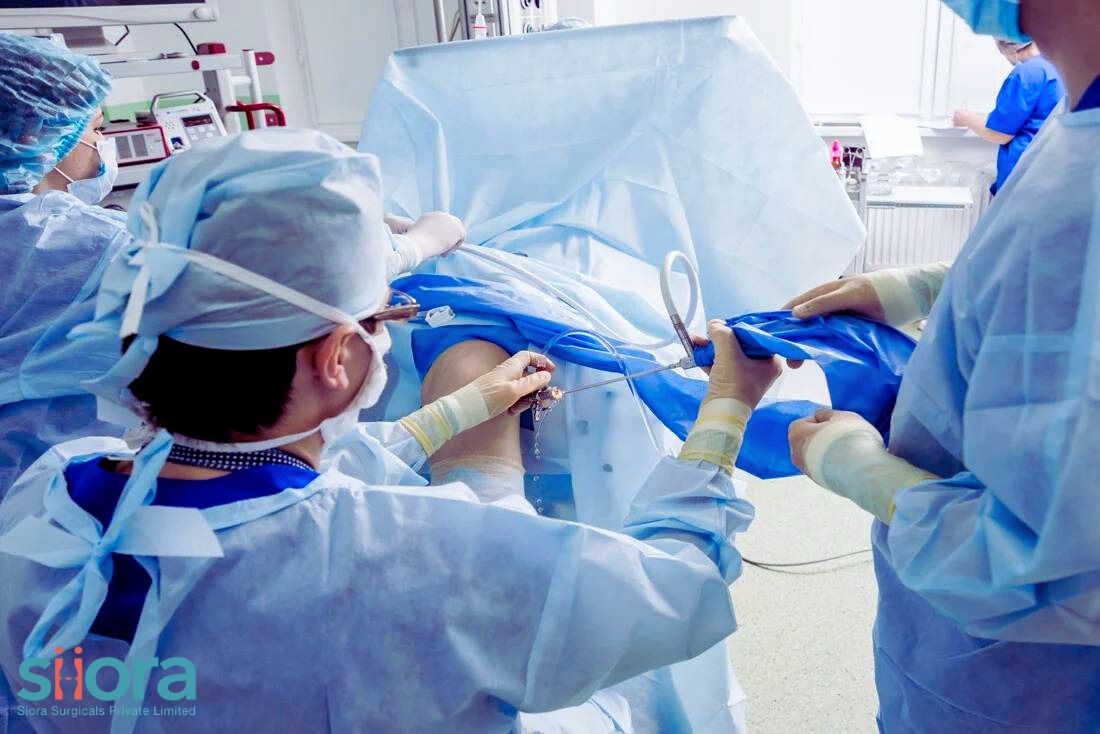
 In the realm of orthopedic medicine, the landscape is continually evolving, with advancements paving the way for more effective and patient-friendly treatments. One notable breakthrough in recent years is the rise of minimally invasive orthopedic procedures. These innovative techniques offer a host of benefits but are not without their share of risks. In this blog, we'll delve into the advantages and potential drawbacks of these procedures, shedding light on the nuanced world of orthopedic care. To get a CE-certified range of minimally invasive orthopedic implants, find experienced Arthroscopy Implants Manufacturers in India. Benefits of Minimally Invasive Orthopedic ProceduresReduced Scarring and Quicker RecoveryOne of the most significant advantages of minimally invasive orthopedic procedures is the minimal impact on the patient's body. Unlike traditional open surgeries that involve large incisions, these procedures use small incisions, resulting in reduced scarring. The smaller incisions contribute to quicker healing times, allowing patients to resume their normal activities sooner. Less Pain and DiscomfortMinimally invasive techniques typically involve less trauma to the surrounding tissues. As a result, patients often experience less pain and discomfort compared to those who undergo traditional open surgeries. This aspect not only enhances the overall patient experience but also reduces the need for prolonged pain management. Shorter Hospital StaysThe nature of minimally invasive procedures allows for shorter hospital stays compared to their open counterparts. Patients can often return home on the same day or after a brief overnight observation, contributing to a faster and more comfortable recovery process. Lower Infection RatesThe risk of postoperative infections is a significant concern in any surgical procedure. Minimally invasive orthopedic procedures, with their smaller incisions, generally result in lower infection rates. This is a crucial advantage that helps improve overall patient safety and lowers the burden on healthcare resources. Risks and ConsiderationsLearning Curve for SurgeonsWhile minimally invasive orthopedic procedures offer numerous benefits, there is a learning curve for surgeons adopting these techniques. Mastering the skills required for precise navigation and control of instruments through small incisions can take time. Surgeons must undergo specialized training to ensure optimal outcomes and minimize the potential for complications. Limited Visibility and AccessThe smaller incisions, while advantageous, also pose challenges in terms of visibility and access to the surgical site. Surgeons must rely on advanced imaging technology and specialized instruments to navigate through tight spaces. In some cases, this limitation may hinder the surgeon's ability to address certain complex conditions effectively. Potential for Nerve and Blood Vessel InjuryThe intricate nature of orthopedic procedures means that there is a potential risk of unintentional damage to nearby nerves and blood vessels. Surgeons must exercise extreme precision to avoid such complications. Additionally, patients must be thoroughly evaluated to ensure that they are suitable candidates for minimally invasive approaches. ConclusionMinimally invasive orthopedic procedures have undoubtedly transformed the landscape of orthopedic care, offering patients a range of benefits, including reduced scarring, quicker recovery, and lower infection rates. However, as with any medical innovation, there are inherent risks that must be carefully considered. Surgeons play a pivotal role in navigating these procedures, requiring specialized skills and training to ensure optimal outcomes. In the ongoing pursuit of enhancing patient care, the careful balance between the benefits and risks of minimally invasive orthopedic procedures remains a critical aspect of the evolving field of orthopedic medicine. Learn about the latest orthopedic procedures & advanced trauma implants and meet renowned industry experts at the AAOS Medical Exhibition in USA.
0 Comments
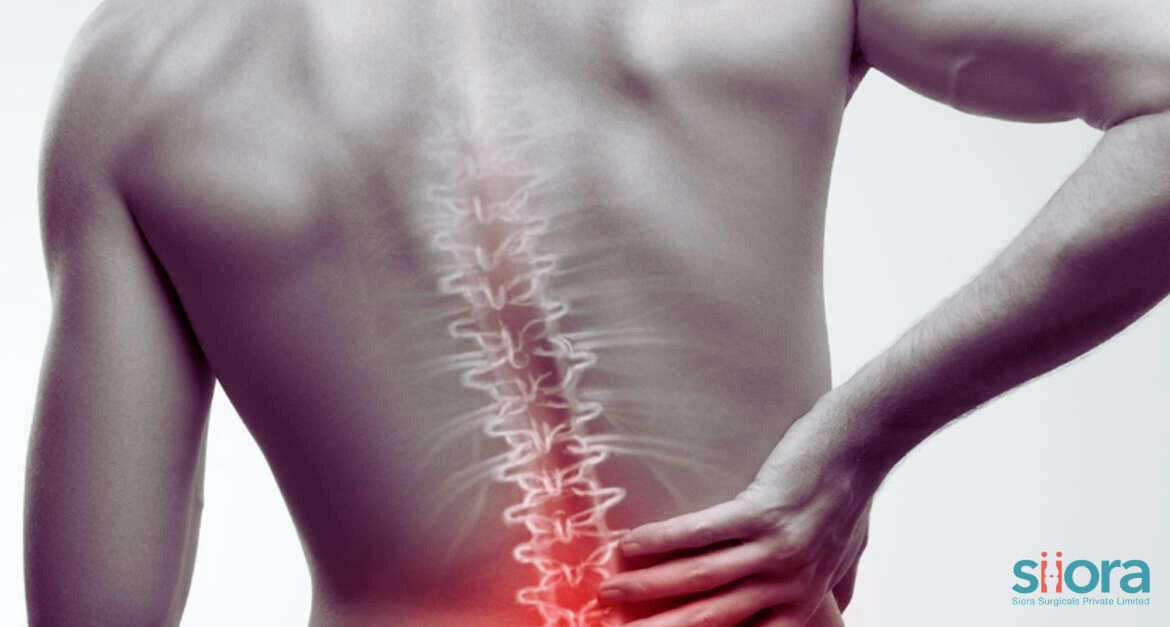 Spinal fractures can be debilitating and life-altering injuries, often requiring a complex and lengthy process of recovery. These injuries can result from a variety of causes, such as accidents, falls, or underlying medical conditions like osteoporosis. Severe spinal fractures demand surgical intervention and, in some cases, the need for Spinal Implants arises. Understanding how recovery from spinal fractures occurs is crucial for patients and their families to navigate this challenging journey toward healing and regaining quality of life. Immediate Medical Attention The recovery process for spinal fractures typically begins with immediate medical attention. When a spinal fracture is suspected or confirmed, emergency medical care is essential to stabilize the injury and prevent further damage. Immobilization of the spine through the use of braces, traction, or surgical intervention may be necessary to ensure the spinal cord is protected and to relieve pain and pressure on the affected area. Diagnostic Imaging After stabilization, diagnostic imaging is performed to assess the extent and severity of the spinal fracture. X-rays, CT scans, and MRI scans are commonly used to visualize the injury and surrounding structures. This step is crucial in determining the appropriate treatment plan and predicting the potential for neurological complications. Non-Surgical Management Depending on the type and severity of the spinal fracture, non-surgical management may be the recommended course of action. This typically involves immobilization with a brace or a cast to allow the fracture to heal naturally. Pain management and physical therapy may also be prescribed to aid in the recovery process. The patient's overall health and the presence of any underlying conditions will influence the choice of treatment. Surgical Intervention In cases where non-surgical methods are inadequate or when the spinal fracture has caused significant instability, surgical intervention may be necessary. Spinal fusion, vertebroplasty, kyphoplasty, and other surgical procedures aim to restore alignment, stabilize the spine, and relieve pressure on the spinal cord and nerves. These surgeries often involve the use of implants such as screws, rods, or cages to maintain spinal stability. Postoperative Recovery The postoperative recovery phase is a critical aspect of the healing process. Patients may need to stay in the hospital for observation and initial rehabilitation. Physical therapy plays a central role in helping patients regain mobility, strength, and function. The rehabilitation program is tailored to the individual and may include exercises to improve posture, flexibility, and core strength. Pain Management Pain management is an essential component of spinal fracture recovery. Patients may experience varying levels of pain, which can hinder their ability to participate in rehabilitation and daily activities. Medications, such as analgesics and anti-inflammatory drugs, are often prescribed to alleviate pain. Additionally, non-pharmacological approaches like heat therapy and transcutaneous electrical nerve stimulation (TENS) can provide relief. Psychological Support Recovery from a spinal fracture can be emotionally taxing. Patients may experience feelings of fear, anxiety, depression, or frustration as they adapt to physical limitations and potential lifestyle changes. Psychological support, including counseling and support groups, can help patients and their families cope with these emotional challenges and provide a sense of hope and resilience. Long-Term Management Recovery from a spinal fracture is not always a quick process. Depending on the severity of the injury, it may take months or even years to achieve maximum recovery. Long-term management involves ongoing monitoring, follow-up appointments, and adjustments to the rehabilitation plan as needed. Patients may also be advised on lifestyle modifications and preventive measures to reduce the risk of future fractures. Building Resilience Spinal fracture recovery is a journey that requires patience, determination, and a strong support system. Building physical and emotional resilience is essential for a successful recovery. Setting realistic goals, maintaining a positive outlook, and adhering to the prescribed treatment plan can make a significant difference in the overall outcome. To know about recent advancements and technologies in the orthopedic industry, visit the 3rd International Conference on Orthopedics in Dubai.  A fracture is a term coined for a broken bone. It can occur due to a variety of factors, such as falls, accidents, or sports injuries. Fractures can be minor or severe, and they can affect any bone in the body. In severe fractures, surgery is required, and it may also involve the use of trauma implants. The healing process for a bone fracture can take several weeks or months. During this time, the body needs a lot of nutrients to help the bone repair itself. A healthy diet can play a key role in supporting fracture healing. The nutrients that are important for fracture healingThere are a number of nutrients that are important for fracture healing. These include: Calcium: Calcium is the main mineral that makes up bones. It is essential for the formation of new bone tissue. Eat plenty of calcium-rich foods. Dairy products, green leafy veggies, and fortified foods are rich in calcium. Vitamin D: Vitamin D is required by the body for the proper absorption of calcium. Get enough of it. You can get vitamin D naturally from sunlight. However, if you don't get enough sunlight, you may need to take a vitamin D supplement. Vitamin K: It is also important for fracture healing. Vitamin K helps the body produce proteins that are needed for bone formation. Protein: Protein is essential for the growth and repair of all tissues in the body, including bones. Good sources of protein include meat, poultry, fish, eggs, dairy products, and beans. Zinc: Zinc is a mineral that helps the body heal wounds and injuries. It is also involved in the production of collagen, which is a protein that is important for bone formation. Include zinc-rich foods in your diet. Good sources of zinc include meat, poultry, fish, eggs, beans, nuts, and seeds. Iron: Iron is a mineral that helps the body carry oxygen to the tissues. It is also important for the production of red blood cells, which are needed for wound healing. Good sources of iron include meat, poultry, fish, beans, lentils, and leafy green vegetables. Potassium: Potassium is a mineral that helps the body maintain fluid balance. It also plays a vital role in muscle function. Good sources of potassium include fruits, vegetables, and whole grains. In addition to eating a healthy diet, it is also important to get enough rest and exercise after a fracture. Rest helps the bone heal, and exercise helps to keep the muscles strong and healthy. Tips for following a healthy diet after a fracture
 Hip replacement surgery is one of the most successful orthopedic surgeries. It is recommended for the treatment of hip joint problems that cannot be managed with conventional non-surgical methods. This surgery involves removing the damaged hip joint and placing a hip prosthesis. Two types of hip replacement surgeries are there, partial hip replacement and total hip replacement. The type of surgery required depends on the severity of the injury and the extent to which the joint is damaged. Now, when it comes to surgeries, there are always risks associated with them along with the benefits. A similar is the case with hip replacement surgery. In this post, we will have a detailed look at the benefits and disadvantages of hip replacement surgery. To get a high-quality range of hip implants, find experienced Orthopedic Medical Device Companies. Pros of Hip Replacement SurgeryHigh Success RateOne of the key advantages of hip replacement surgery is its success rate. Reports have revealed that the success rate of hip replacement surgery is as high as 95% in people with hip pain. Even after 20 years, the success rates boom between 80-85%. This is one of the reasons why orthopedic surgeons don’t hesitate to recommend hip replacement surgery whenever required. Better Hip FunctionIt is seen that people who have undergone hip replacement surgery have experienced better hip function. People after successful hip replacement surgery are able to walk without any discomfort along with other activities that were difficult to perform before surgery. Pain ReliefOne of the reasons for performing hip replacement is to improve pain and it does this perfectly. Total hip replacement surgery is known to significantly reduce pain. In most cases, people experience complete relief from hip pain. Long-Lasting ResultsHip implants are designed to last for long. If we talk about hip replacement surgery, studies have found that in around 80-85 % of cases, implants are still working after 20 years. Cons of Hip Replacement SurgeryInfectionsNot so common but 1% of patients are known to experience bacterial infection around the hip replacement. If not addressed and treated timely, infections can become severe. In some cases, additional surgeries or prolonged antibiotics for treating the infection may be required. Changes in the leg lengthsIt is often noticed that people experience differences in leg lengths after hip replacement surgery. However, the surgeon attempts to keep leg lengths equal, minor differences may occur in order to increase the stability of the hip. DislocationDuring hip replacement surgery, the orthopedic surgeon uses a hip prosthesis to treat the problem. Well, it won’t be wrong to say that it is also prone to dislocation, especially during the initial stages after surgery. Activity LimitationsWell, there is no doubt in saying that hip replacement surgery improves the function and pain in the diseased or injured hip joint. However, it also won’t be wrong to say that there are certain limitations in people with an artificial hip joint. People after hip replacement surgery are advised to avoid rigorous activities like running, putting extra weight on the legs, or sports activities. For a CE-certified range of orthopedic implants contact Siora Surgicals Pvt. Ltd., a leading trauma implants manufacturer in India. The company also exhibits at FIME Show every year. In 2023, you can explore a high-quality range of implants from Siora at booth G41 in FIME. Femoroacetabular Impingement (FAI) is a condition that affects the hip joint, causing pain and limited range of motion. It is characterized by abnormal contact between the femoral head (ball) and the acetabulum (socket) in the hip joint. This article provides an overview of FAI, including its types, causes, symptoms, diagnosis, and treatment options.
To get an international standard quality range of trauma implants, find experienced Orthopedic Instruments Suppliers. Types of Femoroacetabular Impingement FAI can be classified into three main types: pincer, cam, and mixed impingement. Pincer Impingement Pincer impingement occurs when there is excessive coverage of the acetabulum, resulting in the femoral head being compressed. It is typically caused by an overgrown acetabular rim. Cam Impingement Cam impingement is characterized by a non-spherical femoral head shape, causing abnormal contact between the femoral head and the acetabulum. It usually occurs due to a deformity in the neck or head of the femur. Mixed Impingement Mixed impingement refers to a combination of both pincer and cam impingement. It involves abnormalities in both the acetabulum and the femoral head. Causes of Femoroacetabular Impingement FAI can have several causes, including: Developmental Abnormalities Some individuals may develop FAI due to abnormalities in the formation of the hip joint during childhood or adolescence. Genetic Factors Certain genetic factors may contribute to the development of FAI, making some individuals more susceptible to the condition. Overuse or Repetitive Movements Engaging in activities that involve repetitive hip motions or excessive force can lead to FAI over time. Symptoms of Femoroacetabular Impingement The symptoms of FAI can vary among individuals, but common signs include: Hip Pain Patients often experience pain in the groin area, hip joint, or buttocks. The pain may be intermittent or persistent. Limited Range of Motion FAI can restrict hip joint movement, causing stiffness and difficulty with activities like squatting, sitting cross-legged, or flexing the hip. Clicking or Catching Sensation Some individuals may experience a clicking or catching sensation in the hip joint during movement. Diagnosis of Femoroacetabular Impingement To diagnose FAI, a comprehensive evaluation is necessary. The following diagnostic tools and assessments are commonly used: Medical History and Physical Examination The healthcare provider will review the patient's medical history and conduct a physical examination to assess the range of motion of the hip and identify areas of tenderness. Imaging Studies X-rays, magnetic resonance imaging (MRI), or computed tomography (CT) scans can help visualize the hip joint's anatomy and detect abnormalities associated with FAI. Treatment Options for Femoroacetabular Impingement The management of FAI can involve both non-surgical and surgical approaches. Non-Surgical Treatment Non-surgical interventions may include lifestyle modifications, physical therapy, pain management, and activity modification. Surgical Treatment Surgical options for FAI include arthroscopic procedures, such as hip osteoplasty (reshaping of the bone) or labral repair (repairing the cartilage in the hip joint). Conclusion Femoroacetabular Impingement is a condition that can cause hip pain and limited mobility. Understanding the types, causes, symptoms, diagnosis, and treatment options for FAI can help individuals seek appropriate medical care and improve their quality of life. If you suspect you have FAI, it is important to consult an experienced orthopedic specialist. Siora Surgicals Pvt. Ltd. is a renowned orthopedic implant manufacturer in India with over 3 decades of experience in the industry. The company also exhibits at various medical healthcare conferences that take place across the globe. Siora is currently preparing to exhibit at FIME Show 2023. You explore a huge range of orthopedic devices at booth G41 in FIME. Knock knees; also known as Genu Valgum is an orthopedic condition in which the knees of a person touch each other when he/she stands or walk. This may occur either as a developmental/congenital defect or because of a disease or infection. Mild cases of genu valgum may improve without any surgery however, severe cases need surgical intervention. In this post, we will see this condition in detail along with the diagnosis and treatment of the condition.
If you are looking for a CE-certified range of orthopedic implants and instruments, find orthopedic products manufacturers near you. What Are Knock Knees? Knock knees as the name suggests is a condition in which both knees of the person knock against each other. This condition is also characterized by the separation of ankles because of the inward movement of the knees. Knock knees are common in girls but, the condition may also develop in boys. If you know that knock knees are normal in developing kids. Yes, young children have a slight degree of knock knees when they are growing. The condition usually improves until the child grows 6. In some children, it is visible whereas, in some, it is not. In rare cases, an underlying bone disease may also be the cause of knock knees, especially when it develops in the early stages of life. When Knock Knees Become a Problem? You know that knock knees are normal until a certain age. Now, the problem occurs when the curve does not improve after 5 or 6 years of age. Besides this, if it develops after 6 years of age, it is problematic and is known as knock knees syndrome. Knock knees affect both knees however in some cases, the condition may affect only one knee. What Causes Knock Knees? A developmental disease, congenital problem, infection, or traumatic injury may be the cause of knock knees. Here are some of the conditions that may result in genu valgum:
What Are the Symptoms of Knock Knees? One of the most obvious symptoms of knock knees is the separation of the ankles of the person and inward bending of both knees towards each other. A physical examination may easily detect this position of the legs. Besides this, other symptoms of the condition may include:
How Are Knock Knees Diagnosed? The diagnosis of the condition is made with a physical examination followed by imaging tests. During the physical examination, the orthopedic specialist will look for deformity in the leg, especially inward bending of the knees. Besides this, the gait of the person along with other symptoms will also be examined. Diagnostic tests which may be ordered include an x-ray or EOS in standing alignment. What is the Treatment for Knocked Knees? The treatment of the condition will depend on its cause. However, in children, the orthopedic specialist will apply bracing to correct the alignment of the knees. Knee-realignment osteotomy is performed if bracing did not work, or the condition is diagnosed in an adult. If nothing works, surgery is required. During the treatment, the healthcare service provider will also notice the cause of the symptom. For a CE-certified range of orthopedic devices, contact Siora Surgicals Pvt. Ltd., a renowned orthopedic supply company in India. The company is also a regular exhibitor at Florida International Medical Expo, and in 2023, it will exhibit at booth G41 in FIME. Femur is the thighbone, and its long part is known as the femoral shaft. Any fracture occurring in this part is known as a femoral shaft fracture. This is the longest and strongest bone in our body and for a fracture to occur, a strong force is required. A fracture in the femoral shaft often requires surgical intervention and the commonly performed surgical procedure is open reduction and surgical intervention (ORIF). The surgery requires the use of Orthopedic Implant & Instruments,
In this post, we will have a brief look at what femoral shaft fracture is along with its causes and treatment. What Are the Types of Femur Shaft Fractures?Femoral shaft fractures can be of different types depending on the cause and their severity. The pattern of the break in the femoral shaft decides its type. Here are some of the types that are reported: Stable Fractures – The broken pieces of the bone line up correctly Unstable Fractures – The broken pieces are out of their alignment Comminuted Fractures – More than two broken bone fragments are there Open Fractures – The broken bone pierces out of the skin from its sharp end causing significant damage to the skin What Are the Causes of Femoral Shaft Fractures?Young adults are highly at risk of developing femoral shaft fractures because of high-energy trauma like automobile accidents, high-energy collisions, or a direct impact with a solid & heavy object. Besides this, gunshot wounds and falling from a height may also result in femoral shaft fractures. In people with weaker bones like the elderly or those suffering from osteoporosis, low-intensity accidents may also cause femoral shaft fractures. What Are the Symptoms of Fractures in the Femoral Shaft?Intense and immediate pain in the leg is the obvious symptom associated with femoral shaft fractures. Besides this, other symptoms may include:
How Femoral Shaft Fractures Are Diagnosed?The diagnosis of femoral shaft fractures requires both physical examination and imaging tests. At first, the healthcare service provider will thoroughly look for visible signs like swelling and deformity. The patient may also be asked to move the injured leg to examine the range of motion. However, imaging tests are a must to confirm the exact location of the break and its severity. Some of the common imaging tests that healthcare service providers may ask for include:
How Femoral Shaft Fractures Are Treated?Now, when it comes to the treatment of femoral shaft fractures, surgery is required for almost all cases. The commonest surgical procedure that is performed for treating femoral shaft fractures is open reduction and internal fixation (ORIF). This involves the use of large fragment orthopedic implants. In some cases, external fixation is required which involves the use of pins, screws, rods, and an external metal frame. To get a CE-certified range of orthopedic devices including the external fixation system, contact Siora Surgicals Pvt. Ltd., an experienced orthopedic implant manufacturer in India. The company will also exhibit its advanced range of orthopedic devices at FIME Show 2023. You can explore Siora’s range at booth G41 in FIME Miami. Patella (kneecap) is the largest sesamoid bone in our body and it sits above the knee joint. Patella protects the muscles, tendons, and ligaments that form the knee joint and supports various knee movements including bending and straightening of the knee. Patella also protects the knee joint from the daily impacts that the knee experiences.
Sometimes, certain activities or traumatic injuries result in the dislocation of the patella. In severe cases, it breaks. This is a painful condition that makes it difficult for the person to move. As far as the treatment of a fracture is concerned, surgery may be required to realign the broken bone fragments. While on the other hand, a dislocation may be fixed with non-surgical methods along with physical therapy. In this post, we will see how physical therapy helps with patellar dislocation. For a high-quality range of orthopedic devices, contact experienced orthopedic instruments manufacturers. What Are the Types of Patellar Dislocations?Depending on the severity of the cause, patellar dislocations could be of two types:
Patellar Dislocation A dislocation is when the patella completely moves out of its true anatomical position. This could be because of a traumatic event or overuse of the joint. Such cases require immediate medical attention. Patellar Subluxation A subluxation is a condition in which the patella does slip out of its position but is somewhat in contact with its true anatomical position. Sometimes, this condition is also called partial dislocation. What Could Cause Patellar Dislocation?Multiple causes of patellar dislocation are there and the severity of the condition varies based on the cause. Athletes are more prone to patellar dislocations, and this could occur when the knee gets twisted in an awkward position. Besides this, the kneecap also gets dislocated because of a forceful blow to the knee. As a result, the patella moves out of its original position. Above all, another cause of patellar dislocation is weak or tight muscles around the knee joint. How Physical Therapy Helps with the Treatment of Patellar Dislocations?When a kneecap dislocation is suspected, the healthcare service provider will suggest RICE therapy. This involves rest, ice, compression, and elevation. This therapy not only helps improve pain but also controls swelling and inflammation in the knee joint. After this, the orthopedic specialist will also check the position of the patella. If required, the healthcare service provider will realign the kneecap and recommend using crutches or walkers. A period examination of the condition is important to take quick action whenever required. As the healing takes place, the physiotherapist will monitor the condition and suggest exercises to strengthen the joint & soft tissues. Not only this but the physiotherapist will also guide you on how to use crutches effectively. Remember, an initial evaluation of the knee is required before starting the physical therapy and this is what the physiotherapist will do. Siora Surgicals Pvt. Ltd. is an experienced orthopedic device manufacturer in India with over 3 decades in the industry. Along with knee implants, the company produces hundreds of different types of orthopedic devices. Siora is also a regular visitor at various medical health conferences. The company is now preparing to visit Arab Health 2023 in Dubai. There could be multiple causes of hip pain and depending on that, the symptoms and the severity of the condition will be experienced.
If we talk about the term hip pain, then it is a generalized term for the condition characterized by pain in and around the hip. Sometimes, the pain experienced in the groin or thigh is also referred to as hip pain. Depending on the cause and severity, the treatment will be decided. In some cases, fractures cause pain in the hips and surgery may be required for the treatment. In this post, we will see some of the different causes of hip pain along with the treatment required. To get an international standard quality range of hip implants and other orthopedic devices, find experienced Orthopedic Equipment Manufacturers. What Are the Causes of Hip Pain? Some of the common causes of hip pain include: Tendon Inflammation Also known as tendonitis, tendon inflammation is one of the common causes of acute hip pain. If we talk about why this occurs, then too much exercise is to blame. People suffering from tendonitis experience intense pain that improves on its own with time. The condition makes it painful for the person to walk. Arthritis The commonest cause of long-term hip pain is arthritis. Now, the worst part about the condition is that it has no cure, and the treatment provided aims at improving the symptoms. Some of the common causes of arthritis include:
Out of all, osteoarthritis is the most common. The treatment of the condition depends on the type of arthritis and its severity. Besides medication, the healthcare service provider will recommend medications, rest, and physical therapy. Trochanteric Bursitis The inflammation of bursae near the hip joint is known as trochanteric bursitis and it is also of the causes of the hip joint. Postural problems, hip injury, and overuse of the hip joint are among the commonest causes of trochanteric bursitis. The treatment of the condition is provided to reduce inflammation and pain. The doctor may suggest NSAIDs, corticosteroid injections, and physical therapy for the treatment. Surgery will be recommended if required. Hip Fractures Hip fractures are among the common causes of hip pain in older adults. Besides this, fractures are also common in people with osteoporosis. Sudden and severe hip pain is caused by hip fractures. These conditions require immediate medical attention as if delayed, severe complications may occur. Hip fractures generally require surgical intervention to correct fractured bone and bring the pieces back to their original position. This might also involve the use of hip implants. The type of hip implant required depends on the fracture pattern and its severity. For a CE-certified range of orthopedic devices including hip implants¸ contact Siora Surgicals Pvt. Ltd., an experienced orthopedic device manufacturer in India. The company also participates in various Medical Healthcare Conferences and recently, it is preparing to visit Arab Health in Dubai. Open fractures are emergency cases that require immediate assessment by orthopedic experts. These are severe injuries that occur because of high-energy traumas like automobile accidents or gunshots.
These fractures are often treated with internal or external fixation that requires the use of orthopedic implants. Depending on the severity of the fracture, other treatments may also be required. In this post, we will be discussing open fractures in detail along with their investigations and management. If such fractures are left untreated, there will be a high risk of morbidity and mortality. Thus, urgent assessment and management are necessary. PathophysiologyOpen fractures are classifieds as those where the fractured bone protrudes out of the skin and makes direct communication with the external environment. These fractures may be either “in-to-out” or “out-to-in” injuries. This means whether the bone beneath the skin moves out or something penetrates the skin from the outside, like in ballistic injuries or direct blows. The commonest open fractures are the tibial, phalangeal, forearm, metacarpal, and ankle. Clinical Features of Open FracturesThe patient will come with a complaint of pain, swelling, and deformity around the injured area. An overlying wound will be there and in severe cases, the bone may be coming out of the skin. During the examination, it is also necessary to check the neurovascular status along with the tissue loss, if there. The healthcare service provider must also check for contamination at the wound. Diagnosis of Open FracturesThe diagnosis will include a physical examination where the healthcare service provider will check for other injuries to rule out the possibility of life-threatening conditions. It is also important here to know the cause of injury along with the medical history to better identify the right surgery. X-ray examinations and CT scans will also be required to identify damage to the surrounding tissues and the number of breaks. Antibiotic and tetanus injections may also be given to help prevent infection. Treatment of Open FracturesAlmost all open fractures require surgical intervention. It is important to go for surgery as soon as possible to avoid any serious complications. Before the surgical intervention, the healthcare service provider will clean the wound by removing damaged & contaminated tissues and irrigating the wound with a saline solution. After wound cleansing, the surgeon will closely examine the injured site and stabilize the bone. Depending on the severity of the fracture, bone stabilization will be done either with internal or external fixation. Internal Fixation This procedure involves the application of metal plates, rods, & screws to stabilize fractured bone fragments in their true anatomical position while allowing them to heal. This technique is well-suited for fractures with minimal tissue or skin damage and the broken fragments can be well-aligned. External Fixation When it is not feasible to use implants and realign bone fragments, the surgeon will recommend external fixation at first. During this procedure, metal screws and pins are inserted above and below the fracture and they project out of the skin and attached to metal/carbon rods/bars. In some cases, the external fixator is removed, and internal fixation is done after some time. Whereas sometimes the external fixator stays in place until the fracture heals. If you want to participate in an international exhibition and explore advanced medical products and supplies, register for the Tanzania Pharma Expo. Neck pain is a common problem that is noticed in the elderly as well as adults. In most cases, poor postural techniques while doing activities is the cause. If we talk about the elderly, then osteoarthritis may be the cause of neck pain in them. In this post, we will have a look at the causes of neck pain in detail.
For highly orthopedic implants, find experienced orthopedic equipment manufacturers. What Could Cause Neck Pain? Here are the common causes of neck pain you must know: Aging Aging is the cause of most orthopedic conditions and neck pain could be the cause of one of those conditions. With age, the risk of osteoarthritis and spinal stenosis increases. Neck pain could be a symptom of those conditions. Sometimes, stress could lead to the development of a herniated disc or pinched nerve as a result of disc degeneration causing neck pain. Injury Traumatic injuries can affect ligaments, discs, vertebral joints, and nerve roots in the neck region of the spine. A sudden jerk in forward and backward motion during trauma can also be the cause of neck injury. Mental Stress Sometimes, stress can cause muscle tension and result in neck pain and stiffness. Physical Strain Overusing the neck while doing repetitive activities like using the phone for long hours can also cause stiffness and pain in the neck. Conditions that Affect the Spine Poor posture while working in the office, being overweight, and muscle weakness can affect the posture of the spine and as a result, neck pain is experienced. Diseases Diseases like cancer, meningitis, and rheumatoid arthritis can also cause neck pain. How is Neck Pain Diagnosed? The correct diagnosis of neck pain is required to get the right treatment. At first, the healthcare service provider often performs a physical examination to check the visible signs and the range of motion of the neck. Here, the healthcare service provider will pay attention to tenderness, muscle weakness, and numbness. Besides this, the patient will also be asked to move the head forward, backward, and side to side. Now, to confirm the cause, imaging tests will be ordered. The most performed tests may include:
What is the Treatment for Neck Pain?The type of treatment required depends on the cause of neck pain. Although in most cases, self-care and pain medications can provide relief in a week or two. Non-steroidal anti-inflammatory drugs are most commonly prescribed to improve the condition. Sometimes, physical therapy is required. This includes neck-strengthening exercises and correct posture & alignment training. To ease pain, a physiotherapist may also use heat and ice therapy. Transcutaneous electrical nerve stimulation (TENS) therapy is also an option. To relieve severe neck pain, the doctor might give a steroid injection. When it comes to surgery, it is generally not required. If performed, then it is to relieve nerve root or spinal cord compression. To meet hundreds of global healthcare professionals and explore the latest medical technologies and products under one roof, book your visit to the Medical Exhibition Africa. nee pain is a common problem and it may have a number of causes. In some, it can be treated just by medication whereas, in others, more complex treatments are required. Surgery using Ortho Surgical Implants is often the last and only option for the treatment of knee pain when all other methods fail to provide relief.
We are here to discuss some of the available treatment options for knee pain that are used by orthopedic specialists. Knee Pain Treatment Methods Both surgical and non-surgical treatment methods for knee pain are available and we’ll see them one by one. Non-Surgical Methods Pain Medication It won’t be wrong to say that pain-relievers are always the first line of treatment in most cases. Along with prescription drugs, many OTC medicines are also available. But before consuming them, it is advised to consult a specialist. Sometimes, only these medicines are enough to provide long-term relief. Corticosteroid Injections In some cases where pain medication doesn’t work, the doctor may prescribe steroid injections. They are a combination of corticosteroids and anti-inflammatory compounds that are known to provide quick relief from knee pain. These injections are also effective in relieving pain episodes. Platelet-Rich Plasma (PRP) Therapy Platelets are blood components that not only prevent clotting but also promote healing. In PRP therapy, the doctor injects platelet-rich plasma that has been extracted from the patient’s blood into the affected joint. This therapy is being used for treating the pain associated with various joint problems along with sports injuries. A common side effect that may be experienced with this therapy includes temporary inflammation. Knee Brace Knee braces provide support to the knee joint and increase the space in the joint to reduce pressure on the cartilage. Here, it is important to choose the right-size brace or else it can make knee pain worse. Physical Therapy Physical therapy is always the best for relieving pain, improving joint flexibility, and strengthening muscles around the joint. It should be done under the guidance of an expert. Physiotherapy is even required after surgery for improved recovery. Surgical MethodsTotal Knee Replacement Total knee replacement surgery is recommended when the complete joint is damaged as a result of injury or arthritis. During this procedure, the surgeon replaces the damaged joint with a knee implant made of metal or a combination of metal and non-metal. Partial Knee Replacement This surgery is recommended when only a portion is damaged and cannot be repaired by any means. Here, only the damaged part is removed during surgery and a knee implant is placed to complete the knee joint again. One of three knee compartments is replaced during partial knee replacement surgery. Arthroscopic Surgery Arthroscopy is used for the diagnosis as well as the treatment of joint problems. It uses a minimally invasive surgical approach where an arthroscope, a tiny wire with an attached camera is inserted into the joint. Along with this, small orthopedic implants and instruments are also used for the treatment. Osteotomy Osteotomy is performed when wear & tear on one side of the knee is there as a result of poor knee alignment. This method is feasible for physically active individuals and it aims to prevent further progression of knee osteoarthritis. To explore a huge range of medical devices and technologies across various healthcare sectors and meet numerous healthcare professionals, book your visit to the New Medical Show 2022 in Argentina. Arthritis has become a common orthopedic problem in the elderly and the condition can also affect adults. In adults, arthritis may be the cause of traumatic injury. In general, it occurs due to age-related wear & tear of joints that is common with aging. Osteoarthritis is the commonest form of arthritis that affects protective cartilage in our joints. The cartilage not only protects the joints from damage due to impacts but also allows their free & smooth movement. Now, when arthritis results in wear & tear of cartilage, pain, and swelling are a few of the commonly noticed symptoms. Besides this, the affected person also won’t be able to use the joint to its full effect. In severe cases, the joint might not function at all. Such cases may require joint replacement surgery and Knee implants or Hip Replacement Devices may be applied depending on the type of joint affected. The hip joint is among the commonly affected joints by arthritis and in this post, we will be discussing some early and late signs of hip arthritis. What Could Tell You that You might Have Arthritis? The most obvious signs of hip arthritis may include the inability to do routine activities that involve the hip joint. Like, you will find it difficult to stand and sit without pain, walk, bend, and experience persistent pain in the hip joint. Here are some of the signs you may notice: Pain Around the Hip Pain is the commonest symptom of hip arthritis and almost people suffering from the condition might experience mild, moderate, or severe pain in or near the hip. As you know that arthritis is characterized by cartilage damage. Now, if the most-affected area in the hip joint is put under stress, the pain will be severe. Besides this, people suffering from arthritis often experience pain after standing or walking for a long time. Stiffness Another sign of hip arthritis that you might experience is stiffness in the hip. This makes it difficult to move your hip and rotate your leg. Hip stiffness often makes it difficult for you to perform routine activities. Weakness Due to pain in the hip, people often move less, and even for simpler tasks, they rely on others. So, this makes the joint weaker and this worsens symptoms. Sounds While Moving Another common sign of hip arthritis is crackling, snapping, or clicking sounds while standing, sitting, or moving around. If you hear such sounds, it’s time to consult a specialist without wasting much time. How Hip Arthritis can be Treated?Now, you must know that there is no cure for arthritis and the treatment provided only improves symptoms to make the quality of life better. The treatment of hip arthritis depends on its stage and severity of symptoms experienced by the person. In mild to moderate conditions, the doctor often suggests medication to relieve pain & inflammation. Physical therapy is also advised to improve the range of motion of the joint and strengthen muscles. In severe arthritis, joint replacement surgery may be advised. If you are looking to get world-class quality trauma implants, contact Siora Surgicals Pvt. Ltd., a renowned orthopedic device manufacturer in India. The company will also be exhibiting at the FIME Trade Show from 27 to 29th July 2022. Hence, you can also explore a quality range of implants by Siora at the FIME at booth G36. Back pain is a common problem that is not only seen in the elderly but also young adults. Most cases of back pain could have mild causes but, in some cases, the cause could be severe. Spinal problems are known to be the reason for back pain in most cases. Sometimes, the pain becomes so intense and persistent that spinal surgery might be required to relieve pain and other associated symptoms.
To get high-quality spine implants, find reliable and experienced Spinal Implants Manufacturers near you. Surgery is only recommended in cases where back pain caused by spinal issues does not improve with medication or other methods of treatment. While on the other hand, mild to moderate pain can be managed with some simple home remedies. In this post, we will see some tips for managing lower back pain at home. Lower Back Pain Management Tips Be Active Having a sedentary lifestyle is the primary reason for lower back pain. It is often seen that those who keep moving are less likely to experience back pain. Activity is required by our body to burn extra fat, maintain the strength & flexibility of muscles, and perform various biological processes. While on the other hand, a lazy person is highly prone to experiencing various health problems including back pain. Thus, the first and best way to manage lower back pain is to maintain an active lifestyle. Physical Therapy If you are suffering from persistent back pain, physical therapy could help you a lot in improving your condition. Physical therapy helps improve the flexibility of your back muscles while strengthening them and maintaining the natural position of your spine. For this, it is advised to consult a specialist as only he/she could guide you on which exercises you should perform and how much. Maintain Healthy Bodyweight Now, this is something important. Having optimum body weight is the most important as it is among the prime causes of lower back pain. Let us see how. If you are overweight, then your weight is known to put undue stress on your spine and it might start losing its shape. In such cases, lower back pain is likely. While on the other hand, if you are underweight, your bones tend to become weak and so does the spine. Thus, this could also result in lower back pain. So, maintaining ideal body weight is the key to avoiding or improving lower back pain. Keep Body Posture Good Maintaining a good posture of your body while keeping the spine straight could help you in managing backache. For this, you can use tape, stretchy bands, or straps. If not taken care of, the shape of the spine could change a lot and this may cause severe complications later on. So, strictly pay attention to this, or else you might end up in serious trouble. For the content source, contact Siora Surgicals Pvt. Ltd., a reliable orthopedic device manufacturer in India with over 30 years of experience. The company manufactures a CE-certified range of trauma implants and instruments that are also exported to clients based in other countries. Siora is also going to exhibit at FIME Medical Trade Show Miami to gain new opportunities to expand its business and increase brand awareness. Scoliosis is a spinal orthopedic condition that is characterized by the sideways curvature of the spine. This condition is often diagnosed in adolescents. Though scoliosis is common in children, some of the neuromuscular causes like cerebral palsy and muscular dystrophy can make it happen in any life stage.
Most scoliosis cases are known to be mild but, severe conditions may require surgical treatment. In some cases, special spinal implants may also be used. To get high-quality spinal implants, find a reliable Orthopaedic Products Manufacturer near you. In this post, we are going to discuss some of the early signs that indicate the occurrence of scoliosis. Early Signs of Scoliosis If we talk about idiopathic scoliosis, then it is known to start at the age of 10-11 years. It is also noticed that most cases of the condition are mild and do not show any symptoms. As the condition progresses, pain and postural changes in the spine may start. It is often noticed that the abnormal bending of the spine becomes worse during the growth spurt and severe complications may also be seen later on. If the curvature starts worsening, it might also cause breathing difficulties due to the reduction in the space for the lungs to expand properly. A timely diagnosis is necessary to prevent the worsening of the condition. For that, you are advised to take your child to the doctor if you find even slight changes in the body posture or curvature of the spine. If the condition is diagnosed when it is mild, special treatment may not be required as it can be managed with targeted physical therapy and exercises. Surgery to correct the curvature, improve symptoms, and prevent further problems is done in rare cases where the condition is severe and cannot be managed with other treatment methods. Symptoms of Scoliosis
Causes of Scoliosis There are multiple causes of scoliosis while in some cases, no exact cause can be detected. Here are some of the commonly known causes of the condition:
Treatment of Scoliosis The treatment of the condition varies according to the severity and degree of abnormal curve. In most mild cases, no treatment may be required. In such cases, regular check-ups are required to confirm that the condition is not becoming worse. In some cases, the application of braces may keep the spine in its correct position. For severe scoliosis, surgery may be required. The available surgical treatments include:
To get an exceptional range of spinal implants and other orthopedic devices like External Fixator System and Locking Plate for Hand Fracture Titanium, contact Siora Surgicals Pvt. Ltd., an Indian FDA-approved orthopedic device manufacturer. Operating for over 30 years, the company serves hundreds of national and international clients, and Siora always keeps making efforts to increase those numbers. Spondylolisthesis is a spinal condition characterized by slippage of vertebrae onto the one present below. This means the vertebrae move out of their place and sits onto the one below them. When this occurs, the spine becomes unstable, and in such situations, the vertebrae move more than they should. Slipping of the vertebrae may also press on the nerves, and when this occurs, lower back pain or leg pain may be experienced.
Most cases of spondylolisthesis can be treated without surgery whereas, severe cases of the condition may require surgery. The surgical intervention performed to fix this issue requires spinal decompression. This may be performed with or without fusion. If fusion is required, spinal implants may also be applied. For international standard quality spinal implants, find trustworthy Orthopedic Device Companies. In this post, our sole focus will be on discussing spondylolisthesis along with its diagnosis and treatment. What Are the Different Types of Spondylolistheses?Spondylolisthesis can be of many types but, the most common ones include: Congenital Spondylolisthesis This is the form of spondylolisthesis that occurs at the time of birth. In this condition, the spine of the baby does not form as it should in the mother’s womb and that leads to congenital spondylolisthesis. Isthmic Spondylolisthesis This is the form of spondylolisthesis that occurs due to spondylosis. Degenerative Spondylolisthesis This is known as the commonest form of spondylolisthesis as it occurs due to aging. In this form of spondylolisthesis, spinal discs lose water over time. Below mentioned are some of the least common causes of spondylolisthesis: Traumatic Spondylolisthesis This type of spondylolisthesis occurs due to trauma. Post-Surgical Spondylolisthesis As the name suggests, this form of spondylolisthesis is a result of spinal surgery. Pathological Spondylolisthesis Spondylolisthesis can also occur due to osteoporosis and tumors affecting the bone. Who is at the Highest Risk of Developing Spondylolisthesis?Here are certain risk factors that may cause spondylolisthesis: Athletes Young athletes who play sports that involve stretching of the lumbar spine are likely to develop spondylolisthesis. In such cases, growth spurts is the stage in which slippage of the vertebral disc occurs. Genetics In the case of isthmic spondylolisthesis, some people are born with a thinner section of the vertebra known as pars interarticularis. Pars interarticularis connects the facet joints that connect vertebrae from above and below to ensure movement of the spine. This area can fracture or slip in such conditions. Age Age is the common factor that results in degenerative spondylolisthesis. This is when age-related wear & tear weakens the spine, and in such cases, even minor trauma can result in a break or fracture in the spine. This condition is more common after 50 years of age. How Is Spondylolisthesis Diagnosed?Physical examination is the first step during the diagnosis of spondylolisthesis plus, the healthcare service provider also asks about the symptoms experienced by the person. To confirm the diagnosis, certain imaging tests are also required, and they may include:
How is Spondylolisthesis Treated?The treatment of the condition depends upon the grade of slippage of the vertebrae. Besides this, the treatment also depends upon the age of the patient and underlying health conditions, if any. Most cases of the condition can be fixed with non-surgical methods, and they may include:
When it comes to the high-grade treatment of spondylolisthesis, surgery is required. Decompression surgery is often performed, and it may be accompanied by fusion in some cases. If fusion is required, two affected vertebrae are connected. Siora Surgicals Pvt. Ltd. is an experienced orthopedic device manufacturer in India operating for over 30 years. The company specializes in producing an excellent range of orthopedic implants and instruments in stainless steel and titanium. Siora is also looking to expand its market reach by becoming one of the best Orthopedic Equipment Suppliers in Greece. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
November 2023
Categories |
